This post is inspired by the dissection course I led last month. While I have substantial experience in the anatomy lab, being able to direct the curriculum myself is a special privilege I have worked hard to earn.
Anatomy Labs for Yoga Teachers
If you’ve studied with me, you’ve likely heard me say that the study of human anatomy is a lifelong endeavor (hence why I go back to the lab year after year). That said, there are specific structures that attract the attention of yoga teachers. Sometimes this is fame is warranted, but most often it is not. Sometimes the stories are positive, but most often they are not.
These notorious structures (think the “loose” SI joint, the chronically “tight” IT band, the “fragile” knee ligaments, the flexion “intolerant” lumbar spine, etc.) are elusively described in the classroom and poorly depicted in the textbooks. When one has the opportunity to locate, identify, touch, and dissect these structures, the narrative changes quite quickly.
SI Joints, IT Bands, and Knee Ligaments
In my labs, I make a concentrated effort to allow the lab participants to follow their own curiosities while also guiding certain discoveries and promoting conversations relating to biomechanics and pain science in the process.
For example, I make sure anyone who wants to can hold a pelvis and try to move the innominate bones. What they discover is that the innominate bones form a closed loop at the pubis and the sacrum and this loop is extremely secure. We then take specific steps to mechanically “loosen” the loop to no avail. We then speak in depth about how this does not invalidate pain or the sensed experience of an unstable SI joint. It’s one thing to conceptualize this contradiction, it’s another thing to reconcile it for yourself through a hands-on experience.
I also challenge the lab participants to identify the perimeter of the IT band. One would think this is an easy endeavor, but it’s not! Circumferentially, it’s not easy to distinguish from the fascia lata. Longintuntally, it’s not easy to separate from the “insertions”. I find the lab participants fall into two categories here: they either obsess over it until they delineate their version of the solution or they obsess over it while enlisting others to delineate a collective version of the solution. Both are incredible opportunities for learning.
Below, I share with you an image from my book, Yoga Biomechanics: Stretching Redefined, along with an excerpt from the related text, followed by three Thought Provokers. While these aren’t formal “Thought Provokers” you’ll find in the sidebar of the book, they are topics of discussion around the tables in the lab. I’m sharing them with you now so you can ponder them for yourself.
Excerpt from Connectivity and Continuity
(Chapter 4: pgs 115-117)
Joint capsules, which encapsulate the entire joint space, blend into this periosteum layer eventually becoming bone. The inner layer of the joint capsule is the synovial layer, which secretes synovial fluid into the joint space. The outer layer is a fibrous layer that is similar to the fibrous structure of ligaments. In fact, many ligaments are no more than a thickened area of the joint capsule. The knee joint is a good example to use. In the textbooks, the knee is said to have four ligaments – two forming a cross inside the joint space and one running longitudinally on the medial and lateral sides of the joint. The joint capsule is almost always cut away to reveal these two structures and the two within joint space. In vivo, actually, a fibrous band covers the entire joint space, containing the synovial fluid within. Neither the lateral nor medial collateral ligament is separate from the fibrous layer of the joint capsule. Only a very sharp blade and a judgment call by the individual wielding that blade can dissect and identify these “individual” ligaments.
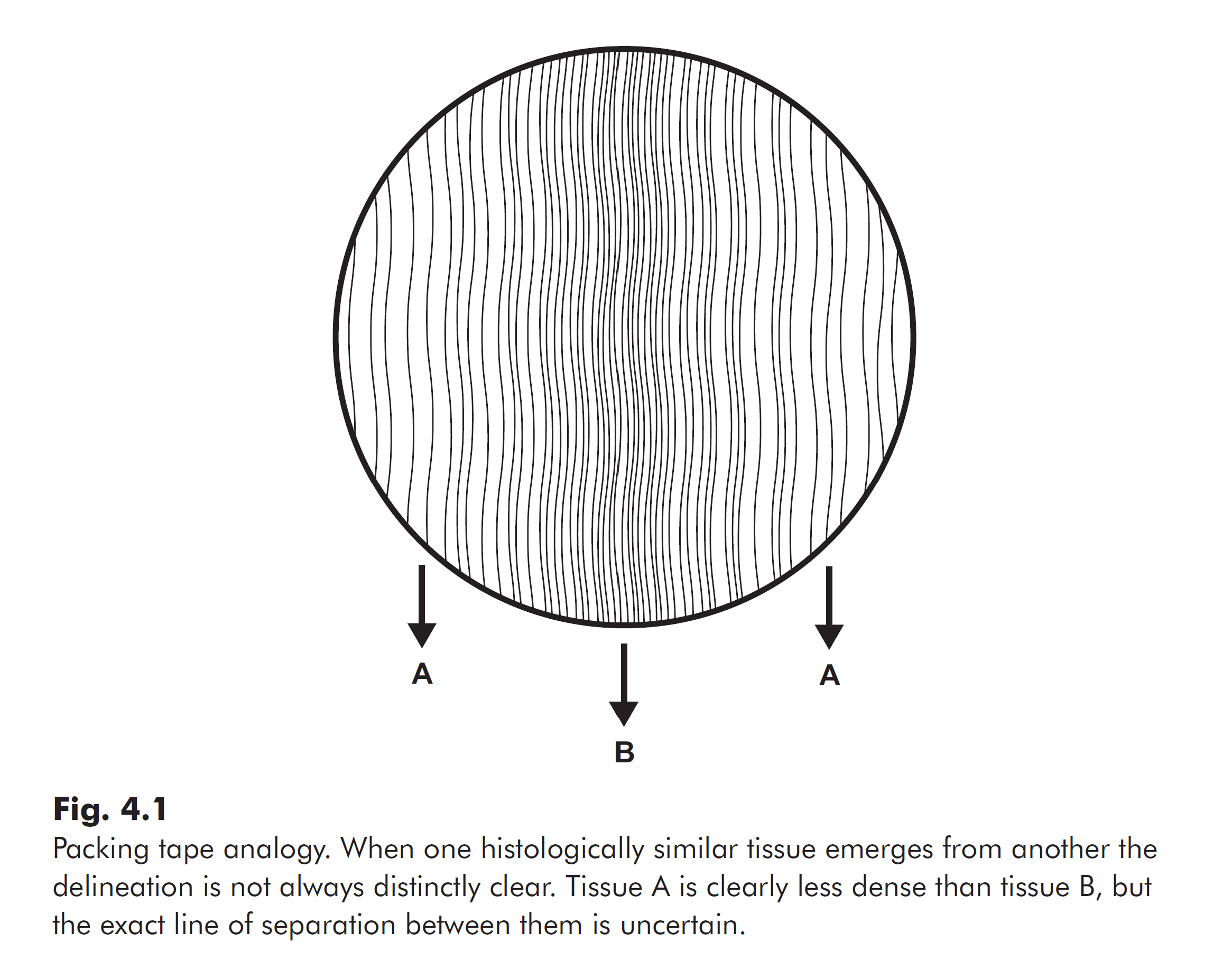
One could say such ligaments are not distinct from joint capsules, but rather emerge from them. To illustrate, imagine the fibrous joint capsule looked something like thick packing tape with parallel threads running through it. If somewhere along the width of the tape, the threads become more densely packed, you could compare the distance between threads to determine the area of greatest concentration to call that a ligament. Another individual, however, may have judged that area to be a millimeter wider. You would both be correct, the distinction is not always that obvious, and that is how similar the structures are.
Explore These 3 Thought Provokers Relating to the Knee
Use these questions to challenge yourself, expand your comfort zone, and stimulate new insights.
Thought Provoker #1:
What has learning the names of the 4 knee ligaments done for your understanding of their function and behavior? How has this translated to the way you protect vs expose the knee from/to certain positions in your classes? How has your study of anatomy so far influenced your understanding of pain? How much of pain is anatomical?
Thought Provoker #2:
What mechanical role do you think the fibrous layer of the joint capsule provides for the knee? Is this in support of or in opposition to the way you studied the ligaments? What is the role of the thickened area we call a ligament? Is this similar or different from the role of the joint capsule? Does stretching affect mechanical behavior and how? Does strengthening affect the mechanical behavior and how? Does hypermobility change the way you answer these questions?
Thought Provoker #3:
When you hear cues like “flex the ankle to protect the knee” (in Figure 4 stretch or single pigeon variations), what does that mean to you? What is the mechanism of action here? What is engaging a specific muscle actually doing to the ligaments and joint capsule? What is it protecting the knee from? Under what conditions is it protective, and under what conditions is it not? How could you study this? What would you measure? If you haven’t heard that cue in particular, what have you heard about the knee in certain yoga poses, and can you apply these same questions?
Comment below with any reflections. I’d love to hear from you.
Extend Your Learning: Anatomy Lab With Jules
HUMAN DISSECTION LAB
4 DAY ANATOMY LAB INTENSIVE
This course is for yoga teachers and committed students who wish to observe the mechanical properties of human connective tissue and get a visual and tactile sense of human movement.
Learn more >

